Living with chronic pain can be a relentless struggle, affecting every aspect of daily life and mental well-being. For those who have not found relief through conventional treatments, advanced pain management solutions like intrathecal pain pump implants offer hope. But what exactly is an intrathecal pain pump implant, and how can it help manage chronic pain effectively?Let’s explore the intricacies of intrathecal pain pumps to understand how they provide targeted, long-term relief for various chronic pain conditions.
Understanding Intrathecal Pain Pumps
An intrathecal pain pump, also known as an intrathecal drug delivery system (IDDS), is a medical device surgically implanted to deliver medication directly into the intrathecal space—the fluid-filled area surrounding the spinal cord. This targeted delivery system allows for precise pain control using smaller medication doses compared to oral administration, minimizing systemic side effects and improving overall quality of life for individuals suffering from chronic pain [1][2].
How Does an Intrathecal Pain Pump Work?
The intrathecal pain pump system comprises two main components:
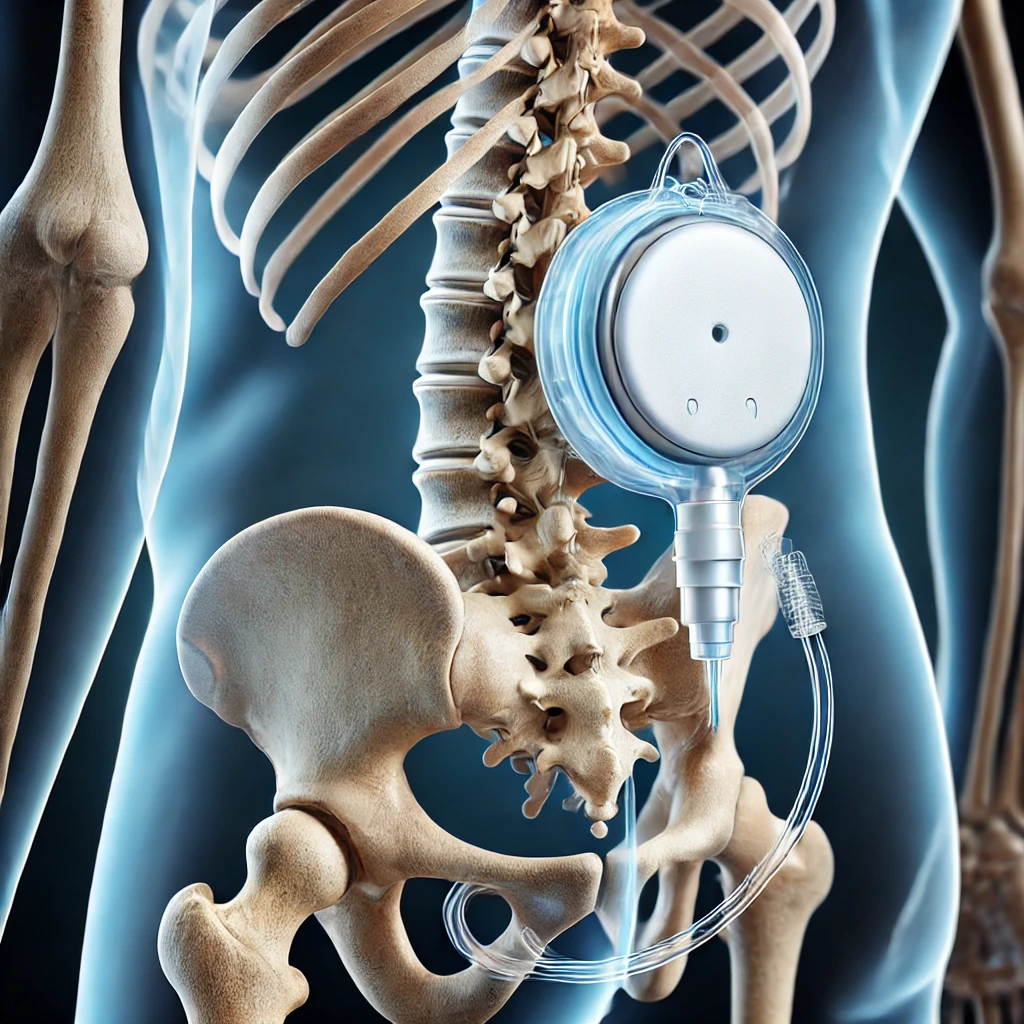
- Pump: A small, programmable device implanted beneath the skin, usually in the abdominal area. It stores and releases prescribed amounts of pain medication at scheduled intervals.
- Catheter: A thin, flexible tube connected to the pump, directing medication into the intrathecal space around the spinal cord.
By delivering medication directly to the central nervous system, the pump effectively blocks pain signals before they reach the brain, providing significant pain relief with reduced medication dosages [3]. Healthcare providers can program and adjust the pump settings externally, tailoring the treatment to the patient’s specific pain needs and lifestyle.
Benefits of Intrathecal Pain Pump Implants
Intrathecal pain pumps offer numerous advantages for individuals struggling with chronic pain:
Targeted and Effective Pain Relief
Delivering medication directly to the spinal cord’s pain receptors ensures more effective pain control, particularly for severe and persistent pain conditions unresponsive to other treatments [2].
Reduced Medication Dosage and Side Effects
The direct delivery method requires significantly lower doses compared to oral medications, reducing the risk of systemic side effects such as drowsiness, nausea, and constipation [4]. This also lowers the potential for dependency and addiction associated with higher-dose oral opioids.
Improved Quality of Life
Patients often experience enhanced mobility, better sleep quality, and increased ability to perform daily activities, leading to overall improved physical and mental well-being [1].
Adjustable and Personalized Treatment
Healthcare providers can easily adjust the pump’s medication type and delivery rate to meet changing pain levels and patient needs, ensuring personalized and adaptable pain management [3].
Long-Term Cost Efficiency
While the initial implantation cost is significant, intrathecal pain pumps can be more cost-effective by reducing hospital visits, medication expenses, and associated healthcare costs related to unmanaged chronic pain [5].
Candidates for Intrathecal Pain Pump Implantation
Intrathecal pain pumps are typically considered for individuals who:
- Suffer from chronic, intractable pain that has not responded to conservative treatments such as oral medications, physical therapy, or less invasive interventions.
- Experience significant side effects from oral pain medications or require high doses for minimal relief.
- Have conditions such as failed back surgery syndrome, complex regional pain syndrome, cancer-related pain, or spasticity disorders like multiple sclerosis and cerebral palsy [2][4].
A thorough evaluation by a pain management specialist is essential to determine suitability. This often includes a trial period where a temporary catheter delivers medication to assess the potential effectiveness and tolerability of the treatment for the patient [3].
The Implantation Procedure
Pre-Procedure Evaluation
Before implantation, patients undergo comprehensive assessments, including medical history reviews, physical examinations, and psychological evaluations. A successful trial infusion demonstrating adequate pain relief is critical before permanent implantation [1].
Surgical Procedure
The implantation involves two main steps performed under local or general anesthesia:
- Catheter Placement: A small incision is made in the back to insert the catheter into the intrathecal space.
- Pump Placement: A second incision is made in the abdomen to create a pocket for the pump. The catheter is then tunneled under the skin and connected to the pump.
The procedure typically takes 1 to 2 hours, and patients may require a short hospital stay for monitoring and initial dose adjustments [5].
Post-Procedure Care
After implantation, regular follow-up appointments are necessary to:
- Refill the pump with medication, usually every few months, depending on dosage and reservoir size.
- Adjust medication dosages and delivery schedules based on pain control effectiveness and patient feedback.
- Monitor for potential complications and ensure the system functions correctly.
Patients are educated on recognizing signs of potential issues and maintaining the device for optimal performance.
Potential Risks and Considerations
While intrathecal pain pumps are generally safe and effective, potential risks and complications include:
- Infection at the implantation site.
- Catheter displacement or blockage leads to inadequate pain control.
- Device malfunction, requiring reprogramming or surgical correction.
- Medication-related side effects, such as respiratory depression, if doses are too high.
Close collaboration with healthcare providers and adherence to follow-up schedules are essential to minimize risks and promptly address complications [4].
Choosing the Right Pain Management Option
Selecting an appropriate pain management strategy is a personalized decision that should be made in consultation with a qualified pain management specialist. Factors to consider include:
- Severity and type of pain.
- Response to previous treatments.
- Overall health status and medical history.
- Lifestyle and personal preferences.
An intrathecal pain pump implant may offer a viable solution for those seeking long-term, effective relief from chronic pain when other treatments have failed. Consulting with a specialist can help determine if this advanced therapy aligns with your pain management goals and improves your quality of life.
Resources:
- Learning About Implanted Pain Pumps for Long-Term Pain. My Health – Alberta[Internet]. Published 2023. Accessed August 21, 2024. Available from: https://myhealth.alberta.ca/Health/aftercareinformation/pages/conditions.aspx?hwid=acl1657
- Understanding the Different Types of Pain Pumps. National Spine & Pain Centers. Published March 4, 2023. Accessed August 21, 2024. Available from: https://www.treatingpain.com/news-updates/2023/march/understanding-the-different-types-of-pain-pumps/
- Intrathecal Pain Pump. Johns Hopkins Medicine [Internet]. Published December 16, 2022. Accessed August 21, 2024. Available from: https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/intrathecal-pain-pump
- Wilkes D. Programmable intrathecal pumps for the management of chronic pain: recommendations for improved efficiency. Journal of Pain Research [Internet]. Published online October 2014:571. doi:https://doi.org/10.2147/jpr.s46929 Accessed August 21, 2024. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4200017/
- Intrathecal Drug Pain Pump Implant | UPMC. UPMC | Life Changing Medicine [Internet]. Accessed August 21, 2024. Available from: https://www.upmc.com/services/neurosurgery/spine/treatment/pain-management/intrathecal-pump
The image shown on the page is AI-generated to show the placement of an intrathecal pain pump implant within the skeleton, highlighting its connection to the spine.